Abstract
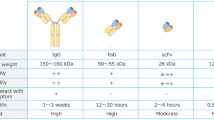
Antibodies, having a high specificity for their particular target, are increasingly being used as therapeutic agents with functions including agonist, antagonist, and targeted drug delivery. The use of many biologic therapies, including antibody fragments, is generally limited by their rapid clearance from plasma. A commonly used approach to extend exposure to biologic therapies is the attachment of polyethylene glycol.
Tumor necrosis factor (TNF)-α is a multifunctional cytokine involved in the regulation of immune responses. Elevated levels of TNFα are found in a wide range of diseases, including the chronic inflammatory conditions rheumatoid arthritis, psoriasis, and Crohn disease (CD). Anti-TNFα antibodies have proved highly efficacious in the treatment of these conditions. In addition, they have proved invaluable for investigating the role of TNFα in disease etiology.
Based on evidence showing that neutralizing antibodies to TNFα were effective in animal models of CD, anti-TNFα antibody treatments were assessed in clinical trials. Interestingly, the anti-TNFα antibody etanercept proved ineffective at achieving remission in active CD despite potently neutralizing soluble TNFα. This indicated that an additional mode of action is also involved in the efficacy of the anti-TNFα agents adalimumab, certolizumab pegol, and infliximab in CD; one suggestion was apoptosis. However, etanercept, like adalimumab and infliximab, can induce apoptosis. Furthermore, certolizumab pegol (which has demonstrated efficacy in CD) does not cause complement-dependent cytotoxicity, antibody-dependent cell-mediated cytotoxicity, apoptosis, or necrosis of neutrophils, all measured in vitro. These functional differences observed with certolizumab pegol stem from its unique structure that does not include the crystallizable fragment (Fc) portion present in the other anti-TNFα agents, and the way in which it signals through membrane TNF.
It is well established that bacteria are a major part of the inflammatory process in CD. The property identified that reflected the efficacies of the anti-TNFα agents etanercept, adalimumab, certolizumab pegol, and infliximab in CD was the ability to inhibit the cytokine production by monocytes that is induced by bacterial lipopolysaccharide. It may therefore be the case that this mode of action is important for efficacy in CD.







Similar content being viewed by others
References
Stockwin LH, Holmes S. Antibodies as therapeutic agents: vive la renaissance! Expert Opin Biol Ther 2003 Oct; 3(7): 1133–52
Lobato MN, Rabbitts TH. Intracellular antibodies and challenges facing their use as therapeutic agents. Trends Mol Med 2003 Sep; 9(9): 390–6
Clark IA. How TNF was recognized as a key mechanism of disease. Cytokine Growth Factor Rev 2007 Jun–Aug; 18(3–4): 335–43
Holliger P, Hudson PJ. Engineered antibody fragments and the rise of single domains. Nat Biotechnol 2005 Sep; 23(9): 1126–36
Weir AN, Nesbitt A, Chapman AP, et al. Formatting antibody fragments to mediate specific therapeutic functions. Biochem Soc Trans 2002 Aug; 30(4): 512–6
Caliceti P, Veronese FM. Pharmacokinetic and biodistribution properties of poly(ethylene glycol)-protein conjugates. Adv Drug Deliv Rev 2003 Sep 26; 55(10): 1261–77
Aggarwal BB. Signalling pathways of the TNF superfamily: a double-edged sword. Nat Rev Immunol 2003 Sep; 3(9): 745–56
Watts AD, Hunt NH, Wanigasekara Y, et al. A casein kinase I motif present in the cytoplasmic domain of the tumour necrosis factor ligand family is implicated in ‘reverse signaling’. EMBO J 1999 Apr; 18(8): 2119–26
Loftus EV, Schoenfeld P, Sandborn WJ. The epidemiology and natural history of Crohn’s disease in population-based patient cohorts from North America: a systematic review. Aliment Pharmacol Ther 2002 Jan; 16(1): 51–60
Bernstein CN. The epidemiology of inflammatory bowel disease in Canada: a population-based study. Am J Gastroenterol 2006 Jan; 101(7): 1559–68
Sands BE. Inflammatory bowel disease: past, present, and future. J Gastroenterol 2007 Jan; 42: 16–25
Van Deventer SJ. Tumour necrosis factor and Crohn’s disease. Gut 1997 Apr; 40: 443–8
Van Dullemen HM, van Deventer SJ, Hommes DW, et al. Treatment of Crohn’s disease with anti-tumour necrosis factor chimeric antibody (cA2). Gastroenterology 1995 Jul; 109(1): 129–35
Targan SR, Hanauer SB, van Deventer SJH, et al. A short-term study of chimeric monoclonal antibody cA2 to tumor necrosis factor α for Crohn’s disease. N Engl J Med 1997 Oct; 337(15): 1029–35
Present DH, Rutgeerts P, Targan S, et al. Infliximab for the treatment of fistulas in patients with Crohn’s disease. N Engl J Med 1999 May; 340: 1398–405
Rutgeerts P, D’Haens G, Targan S, et al. Efficacy and safety of retreatment with anti-tumour necrosis factor antibody (infliximab) to maintain remission in Crohn’s disease. Gastroenterology 1999; 117: 761–9
Sandborn WJ, Hanauer SB, Katz S, et al. Etanercept for active Crohn’s disease: a randomised, double-blind, placebo-controlled trial. Gastroenterology 2001 Nov; 121: 1088–94
Baker M, Stringer F, Stephens S. Pharmacokinetic properties of the anti-TNF agent certolizumab pegol [abstract]. Gut 2006; 55Suppl. V: A122
Sandborn WJ, Feagan BG, Stoinov S, et al., for the PRECISE 1 Study Investigators. Certolizumab pegol for the treatment of Crohn’s disease. N Engl J Med 2007; 357: 228–38
Schreiber S, Khaliq-Kareemi M, Lawrance IC, et al., for the PRECISE 2 Study Investigators. Maintenance therapy with certolizumab pegol for Crohn’s disease. N Engl J Med 2007; 357: 239–50
Chapman AP. PEGylated antibodies and antibody fragments for improved therapy: a review. Adv Drug Deliv Rev 2002; 54: 531–45
Smith B, Ceska T, Henry A, et al. Detailing the novel structure of the biopharma-ceutical certolizumab pegol [abstract]. J Crohn’s Colitis 2008; 2(1): 50
Lugering A, Schmidt M, Lugering N, et al. Infliximab induces apoptosis in monocytes from patients with chronic active Crohn’s disease by using a caspase-dependent pathway. Gastroenterology 2001 Nov; 121: 1145–57
Shen C, Assche GV, Colpaert S, et al. Adalimumab induces apoptosis of human monocytes: a comparative study with infliximab and etanercept. Aliment Pharmacol Ther 2005 Feb; 21: 251–8
Van den Brande JM, Braat H, van den Brink GR, et al. Infliximab but not etanercept induced apoptosis in lamina propria T-lymphocytes from patients with Crohn’s disease. Gastroenterology 2003 Jun; 124: 1774–85
ten Hove T, van Montfrans C, Peppelenbosch MP, et al. Infliximab treatment induces apoptosis of lamina propria T lymphocytes in Crohn’s disease. Gut 2002 Feb; 50: 206–11
Scallon BJ, Moore MA, Trinh H, et al. Chimeric anti-TNFα monoclonal antibody cA2 binds recombinant transmembrane TNFα and activates immune effector functions. Cytokine 1995 Apr; 7: 251–9
Kirchner S, Holler E, Haffner S, et al. Effect of different tumor necrosis factor (TNF) reactive agents on reverse signaling of membrane integrated TNF in monocytes. Cytokine 2004 Oct; 28: 67–74
Nesbitt A, Fossati G, Bergin M, et al. Mechanism of action of certolizumab pegol (CDP870): in vitro comparison with other anti-tumor necrosis factor alpha agents. Inflamm Bowel Dis 2007; 13: 1323–32
Mpofu S, Fatima F, Moots RJ. Anti-TNF-α therapies: they are all the same (aren’t they?). Rheumatology 2005 Mar; 44: 271–3
Mitoma H, Horiuchi T, Hatta N, et al. Infliximab induces potent anti-inflammatory responses by outside-to-inside signals through transmembrane TNF-α. Gastroenterology 2005 Feb; 128: 376–92
Eissner G, Kirchner S, Lindner H, et al. Reverse signaling through transmembrane TNF confers resistance to lipopolysaccharide in human monocytes and macrophages. J Immunol 2000 Jun; 164: 6193–8
Ringheanu M, Daum F, Markowitz J, et al. Effects of infliximab on apoptosis and reverse signaling of monocytes from healthy individuals and patients with Crohn’s disease. Inflam Bowel Dis 2004 Nov; 10(6): 801–10
Xin L, Wang J, Zhang H, et al. Dual regulation of soluble tumor necrosis factor-α induced activation of human monocytic cells via modulating transmembrane TNF-α-mediated ‘reverse signalling’. Int J Mol Med 2006 Nov; 18: 885–92
Acknowledgments
T. Bourne, A. Nesbitt, and G. Fossati are employees of UCB. The work described was also funded by UCB.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bourne, T., Fossati, G. & Nesbitt, A. A PEGylated Fab’ Fragment against Tumor Necrosis Factor for the Treatment of Crohn Disease. BioDrugs 22, 331–337 (2008). https://doi.org/10.2165/00063030-200822050-00005
Published:
Issue Date:
DOI: https://doi.org/10.2165/00063030-200822050-00005