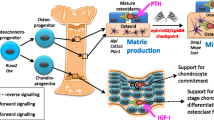
Abstract
The understanding of cell interactions and genetic controls of bone cells has provided new approaches to drug development for osteoporosis. Current emphasis in the development of new anabolic therapies is directed at modifying the effects of Wnt signalling on osteoblast differentiation and bone formation. Local signalling that results in bone formation during remodelling takes place in several ways. Growth factors released from resorbed bone matrix can contribute to preosteoblast differentiation and bone formation. Osteoclasts in the bone multicellular units (BMUs) might also generate activity that contributes to bone formation. The preosteoblasts themselves, growing in the resorption space, can communicate through cell contact and paracrine signalling mechanisms to differentiate. Osteocytes can sense the need for bone repair by detecting damage and pressure changes, and signalling to surface cells to respond appropriately. These recent insights into cell communication, together with discoveries from human and mouse genetics, have opened new pathways to drug development for osteoporosis. With the anabolic effect of parathyroid hormone on the skeleton having been established, human genetics revealed the major role of Wnt signalling in bone formation, and this has become the target of activity. Current approaches include activation at any of several points in the Wnt pathway, and neutralization of sclerostin, the protein product of the SOST gene that is produced in osteocytes as a powerful inhibitor of bone formation.


Similar content being viewed by others
References
Delmas PD (2002) Treatment of postmenopausal osteoporosis. Lancet 359:2018–2026
Parfitt AM (1996) Skeletal heterogeneity and the purposes of bone remodelling: implications for the understanding of osteoporosis. In: Marcus R, Feldman D, Kelsey J (eds) Osteoporosis. Academic, San Diego, pp 315–339
Seeman E, Delmas PD (2006) Bone quality—the material and structural basis of bone strength and fragility. N Engl J Med 354:2250–2261
Van der Linden JC, Homminga J, Verhaar JA, Weinans H (2001) Mechanical consequences of bone loss in cancellous bone. J Bone Miner Res 16:457–465
Hauge EM, Qvesel D, Eriksen EF, Mosekilde L, Melsen F (2001) Cancellous bone remodeling occurs in specialized compartments lined by cells expressing osteoblastic markers. J Bone Miner Res 16:1575–1582
Eriksen EF, Eghbali-Fatourechi GZ, Khosla S (2007) Remodeling and vascular spaces in bone. J Bone Miner Res 22:1–6
Eghbali-Fatourechi GZ, Lamsam J, Fraser D, Nagel D, Riggs BL, Khosla S (2005) Circulating osteoblast-lineage cells in humans. N Engl J Med 352:1959–1966
Modder UI, Khosla S (2008) Skeletal stem/osteoprogenitor cells: current concepts, alternate hypotheses, and relationship to the bone remodeling compartment. J Cell Biochem 103(2):393–400
Neer RM, Arnaud CD, Zanchetta JR et al (2001) Effect of parathyroid hormone (1–34) on fractures and bone mineral density in postmenopausal women with osteoporosis. N Engl J Med 344:1434–1441
Lips P, Courpron P, Meunier PJ (1978) Mean wall thickness of trabecular bone packets in the human iliac crest: changes with age. Calcif Tissue Res 26:13–17
Vedi S, Compston JE, Webb A, Tighe JR (1982) Histomorphometric analysis of bone biopsies from the iliac crest of normal British subjects. Metab Bone Dis Relat Res 4:231–236
Bikle DD, Sakata T, Leary C et al (2002) Insulin-like growth factor I is required for the anabolic actions of parathyroid hormone on mouse bone. J Bone Miner Res 17:1570–1578
Miyakoshi N, Kasukawa Y, Linkhart TA, Baylink DJ, Mohan S (2001) Evidence that anabolic effects of PTH on bone require IGF-I in growing mice. Endocrinology 142:4349–4356
Zhang M, Xuan S, Bouxsein MLet al (2002) Osteoblast-specific knockout of the insulin-like growth factor (IGF) receptor gene reveals an essential role of IGF signalling in bone matrix mineralization. J Biol Chem 277:44005–44012
Wang Y, Nishida S, Boudignon BM et al (2007) IGF-I receptor is required for the anabolic actions of parathyroid hormone on bone. J Bone Miner Res 22:1329–1337
Ebeling PR, Jones JD, O’Fallon WM, Janes CH, Riggs BL (1993) Short-term effects of recombinant human insulin-like growth factor I on bone turnover in normal women. J Clin Endocrinol Metab 77:1384–1387
Jilka RL, Weinstein RS, Bellido T, Roberson P, Parfitt AM, Manolagas SC (1999) Increased bone formation by prevention of osteoblast apoptosis with parathyroid hormone. J Clin Invest 104:439–446
Jilka RL, Weinstein RS, Parfitt AM, Manolagas SC (2007) Quantifying osteoblast and osteocyte apoptosis: challenges and rewards. J Bone Miner Res 22:1492–1501
Miao D, He B, Jiang Y et al (2005) Osteoblast-derived PTHrP is a potent endogenous bone anabolic agent that modifies the therapeutic efficacy of administered PTH 1–34. J Clin Invest 115:2402–2411
Zhao G, Monier-Faugere MC, Langub MC et al (2000) Targeted overexpression of insulin-like growth factor I to osteoblasts of transgenic mice: increased trabecular bone volume without increased osteoblast proliferation. Endocrinology 141:2674–2682
Weinstein RS, Jilka RL, Parfitt AM, Manolagas SC (1998) Inhibition of osteoblastogenesis and promotion of apoptosis of osteoblasts and osteocytes by glucocorticoids. Potential mechanisms of their deleterious effects on bone. J Clin Invest 102:274–282
Karsenty G (2001) Minireview: transcriptional control of osteoblast differentiation. Endocrinology 142:2731–2733
Ducy P, Starbuck M, Priemel M et al (1999) A Cbfa1-dependent genetic pathway controls bone formation beyond embryonic development. Genes Dev 13:1025–1036
Krishnan V, Moore TL, Ma YL et al (2003) Parathyroid hormone bone anabolic action requires Cbfa1/Runx2-dependent signalling. Mol Endocrinol 17:423–435
Geoffroy V, Kneissel M, Fournier B, Boyde A, Matthias P (2002) High bone resorption in adult aging transgenic mice overexpressing cbfa1/runx2 in cells of the osteoblastic lineage. Mol Cell Biol 22:6222–6233
Nakashima K, Zhou X, Kunkel G et al (2002) The novel zinc finger-containing transcription factor osterix is required for osteoblast differentiation and bone formation. Cell 108:17–29
Compston JE (2007) Skeletal actions of intermittent parathyroid hormone: effects on bone remodelling and structure. Bone 40:1447–1452
Jilka RL (2007) Molecular and cellular mechanisms of the anabolic effect of intermittent PTH. Bone 40:1434–1446
Frolik CA, Black EC, Cain RL et al (2003) Anabolic and catabolic bone effects of human parathyroid hormone (1–34) are predicted by duration of hormone exposure. Bone 33:372–379
Dobnig H, Turner RT (1995) Evidence that intermittent treatment with parathyroid hormone increases bone formation in adult rats by activation of bone lining cells. Endocrinology 136:3632–3638
Bellido T, Ali AA, Plotkin LI et al (2003) Proteasomal degradation of Runx2 shortens parathyroid hormone-induced anti-apoptotic signalling in osteoblasts. A putative explanation for why intermittent administration is needed for bone anabolism. J Biol Chem 278:50259–50272
Bellido T, Ali AA, Gubrij I et al (2005) Chronic elevation of parathyroid hormone in mice reduces expression of sclerostin by osteocytes: a novel mechanism for hormonal control of osteoblastogenesis. Endocrinology 146:4577–4583
Shoback DM, Bilezikian JP, Turner SA, McCary LC, Guo MD, Peacock M (2003) The calcimimetic cinacalcet normalizes serum calcium in subjects with primary hyperparathyroidism. J Clin Endocrinol Metab 88:5644–5649
Nemeth EF, Delmar EG, Heaton WL et al (2001) Calcilytic compounds: potent and selective Ca2+ receptor antagonists that stimulate secretion of parathyroid hormone. J Pharmacol Exp Ther 299:323–331
Gowen M, Stroup GB, Dodds RA et al (2000) Antagonizing the parathyroid calcium receptor stimulates parathyroid hormone secretion and bone formation in osteopenic rats. J Clin Invest 105:1595–1604
Kumar S, Liang X, Vasko JA et al (2007) Oral treatment with calcium receptor antagonist SB-423557 causes PTH release in multiple species and positive bone forming effects in the rat. J Bone Miner Res 22:S88
Ethgen D, Danoff, Schultz et al (2007) Antagonism of a calcium sensing receptor stimulates dose-related release of endogenous parathyroid hormone in normal volunteers: a proof of concept study. J Bone Miner Res 22:S128
Ethgen D, Phillips JC, Matheny C et al (2007) Dose-dependent increases in endogenous parathyroid hormone concentration after administration of a calcium-sensing receptor antagonist to normal volunteers for an oral bone forming agent. J Bone Miner Res 22:S38
Philbrick WM, Wysolmerski JJ, Galbraith S (1996) Defining the roles of parathyroid hormone-related protein in normal physiology. Physiol Rev 76:127–173
Martin TJ, Moseley JM, Williams ED (1997) Parathyroid hormone-related protein: hormone and cytokine. J Endocrinol 154 [Suppl]:S23–S37
Hock JM, Fonseca J, Gunness-Hey M, Kemp BE, Martin TJ (1989) Comparison of the anabolic effects of synthetic parathyroid hormone-related protein (PTHrP) 1–34 and PTH 1–34 on bone in rats. Endocrinology 125:2022–2027
Everhart-Caye M, Inzucchi SE, Guinness-Henry J, Mitnick MA, Stewart AF (1996) Parathyroid hormone (PTH)-related protein(1–36) is equipotent to PTH(1–34) in humans. J Clin Endocrinol Metab 81:199–208
Horwitz MJ, Tedesco MB, Gundberg C, Garcia-Ocana A, Stewart AF (2003) Short-term, high-dose parathyroid hormone-related protein as a skeletal anabolic agent for the treatment of postmenopausal osteoporosis. J Clin Endocrinol Metab 88:569–575
Hodsman AB, Steer BM (1993) Early histomorphometric changes in response to parathyroid hormone therapy in osteoporosis: evidence for de novo bone formation on quiescent cancellous surfaces. Bone 14:523–527
Kostenuik PJ, Ferrari S, Pierroz D et al (2007) Infrequent delivery of a long-acting PTH-Fc fusion protein has potent anabolic effects on cortical and cancellous bone. J Bone Miner Res 22:1534–1547
Amizuka N, Warshawsky H, Henderson JE, Goltzman D, Karaplis AC (1994) Parathyroid hormone-related peptide-depleted mice show abnormal epiphyseal cartilage development and altered endochondral bone formation. J Cell Biol 126:1611–1623
Kartsogiannis V, Moseley J, McKelvie B et al (1997) Temporal expression of PTHrP during endochondral bone formation in mouse and intramembranous bone formation in an in vivo rabbit model. Bone 21:385–392
Suda N, Gillespie MT, Traianedes K et al (1996) Expression of parathyroid hormone-related protein in cells of osteoblast lineage. J Cell Physiol 166:94–104
Amizuka N, Karaplis AC, Henderson JE (1996) Haploinsufficiency of parathyroid hormone-related peptide (PTHrP) results in abnormal postnatal bone development. Dev Biol 175:166–176
Jiang Y, Zhao JJ, Mitlak BH, Wang O, Genant HK, Eriksen EF (2003) Recombinant human parathyroid hormone (1–34) [teriparatide] improves both cortical and cancellous bone structure. J Bone Miner Res 18:1932–1941
Seeman E, Delmas PD (2001) Reconstructing the skeleton with intermittent parathyroid hormone. Trends Endocrinol Metab 12:281–283
Martin TJ, Sims NA (2005) Osteoclast-derived activity in the coupling of bone formation to resorption. Trends Mol Med 11:76–81
Karsdal MA, Martin TJ, Bollerslev J, Christiansen C, Henriksen K (2007) Are nonresorbing osteoclasts sources of bone anabolic activity? J Bone Miner Res 22:487–494
Lindsay R, Cosman F, Zhou H et al (2006) A novel tetracycline labeling schedule for longitudinal evaluation of the short-term effects of anabolic therapy with a single iliac crest bone biopsy: early actions of teriparatide. J Bone Miner Res 21:366–373
Dobnig H, Sipos A, Jiang Y et al (2005) Early changes in biochemical markers of bone formation correlate with improvements in bone structure during teriparatide therapy. J Clin Endocrinol Metab 90:3970–3977
Koh AJ, Demiralp B, Neiva KG et al (2005) Cells of the osteoclast lineage as mediators of the anabolic actions of parathyroid hormone in bone. Endocrinology 146:4584–4596
Delmas PD, Seeman E (2004) Changes in bone mineral density explain little of the reduction in vertebral or nonvertebral fracture risk with anti-resorptive therapy. Bone 34:599–604
Sarkar S, Mitlak BH, Wong M, Stock JL, Black DM, Harper KD (2002) Relationships between bone mineral density and incident vertebral fracture risk with raloxifene therapy. J Bone Miner Res 17:1–10
Ettinger B, San Martin J, Crans G, Pavo I (2004) Differential effects of teriparatide on BMD after treatment with raloxifene or alendronate. J Bone Miner Res 19:745–751
Black DM, Greenspan SL, Ensrud KE et al (2003) The effects of parathyroid hormone and alendronate alone or in combination in postmenopausal osteoporosis. N Engl J Med 349:1207–1215
Finkelstein JS, Hayes A, Hunzelman JL, Wyland JJ, Lee H, Neer RM (2003) The effects of parathyroid hormone, alendronate, or both in men with osteoporosis. N Engl J Med 349:1216–1226
Cosman F, Nieves J, Zion M, Woelfert L, Luckey M, Lindsay R (2005) Daily and cyclic parathyroid hormone in women receiving alendronate. N Engl J Med 353:566–575
Martin TJ (2004) Does bone resorption inhibition affect the anabolic response to parathyroid hormone? Trends Endocrinol Metab 15:49–50
Black DM, Bilezikian JP, Ensrud KE et al (2005) One year of alendronate after one year of parathyroid hormone (1–84) for osteoporosis. N Engl J Med 353:555–565
Wodarz A, Nusse R (1998) Mechanisms of Wnt signalling in development. Annu Rev Cell Dev Biol 14:59–88
Uusitalo M, Heikkila M, Vainio S (1999) Molecular genetic studies of Wnt signalling in the mouse. Exp Cell Res 253:336–348
Westendorf JJ, Kahler RA, Schroeder TM (2004) Wnt signalling in osteoblasts and bone diseases. Gene 341:19–39
Clevers H (2006) Wnt/beta-catenin signalling in development and disease. Cell 127:469–480
Yang-Snyder J, Miller JR, Brown JD, Lai CJ, Moon RT (1996) A frizzled homolog functions in a vertebrate Wnt signalling pathway. Curr Biol 6:1302–1306
Slusarski DC, Corces VG, Moon RT (1997) Interaction of Wnt and a Frizzled homologue triggers G-protein-linked phosphatidylinositol signalling. Nature 390:410–413
He X, Saint-Jeannet JP, Wang Y, Nathans J, Dawid I, Varmus H (1997) A member of the Frizzled protein family mediating axis induction by Wnt-5A. Science 275:1652–1654
Hsieh JC, Rattner A, Smallwood PM, Nathans J (1999) Biochemical characterization of Wnt-frizzled interactions using a soluble, biologically active vertebrate Wnt protein. Proc Natl Acad Sci USA 96:3546–3551
Pinson KI, Brennan J, Monkley S, Avery BJ, Skarnes WC (2000) An LDL-receptor-related protein mediates Wnt signalling in mice. Nature 407:535–538
Mao B, Wu W, Li Y et al (2001) LDL-receptor-related protein 6 is a receptor for Dickkopf proteins. Nature 411:321–325
Mao J, Wang J, Liu B et al (2001) Low-density lipoprotein receptor-related protein-5 binds to Axin and regulates the canonical Wnt signalling pathway. Mol Cell 7:801–809
Gong Y, Slee RB, Fukai N et al (2001) LDL receptor-related protein 5 (LRP5) affects bone accrual and eye development. Cell 107:513–523
Boyden LM, Mao J, Belsky J et al (2002) High bone density due to a mutation in LDL-receptor-related protein 5. N Engl J Med 346:1513–1521
Mani A, Radhakrishnan J, Wang H et al (2007) LRP6 mutation in a family with early coronary disease and metabolic risk factors. Science 315:1278–1282
Balemans W, Van Hul W (2007) The genetics of low-density lipoprotein receptor-related protein 5 in bone: a story of extremes. Endocrinology 148:2622–2629
Li J, Sarosi I, Cattley RC et al (2006) Dkk1-mediated inhibition of Wnt signalling in bone results in osteopenia. Bone 39:754–766
Kato M, Patel MS, Levasseur R et al (2002) Cbfa1-independent decrease in osteoblast proliferation, osteopenia, and persistent embryonic eye vascularization in mice deficient in Lrp5, a Wnt coreceptor. J Cell Biol 157:303–314
Babij P, Zhao W, Small C et al (2003) High bone mass in mice expressing a mutant LRP5 gene. J Bone Miner Res 18:960–974
Rawadi G, Vayssiere B, Dunn F, Baron R, Roman-Roman S (2003) BMP-2 controls alkaline phosphatase expression and osteoblast mineralization by a Wnt autocrine loop. J Bone Miner Res 18:1842–1853
Johnson ML, Harnish K, Nusse R, Van Hul W (2004) LRP5 and Wnt signalling: a union made for bone. J Bone Miner Res 19:1749–1757
Mbalaviele G, Sheikh S, Stains JP et al (2005) Beta-catenin and BMP-2 synergize to promote osteoblast differentiation and new bone formation. J Cell Biochem 94:403–418
Tu X, Joeng KS, Nakayama KI et al (2007) Noncanonical Wnt signalling through G protein-linked PKCdelta activation promotes bone formation. Dev Cell 12:113–127
Takada I, Mihara M, Suzawa M et al (2007) A histone lysine methyltransferase activated by non-canonical Wnt signalling suppresses PPAR-gamma transactivation. Nat Cell Biol 9:1273–1285
Balemans W, Ebeling M, Patel N et al (2001) Increased bone density in sclerosteosis is due to the deficiency of a novel secreted protein (SOST). Hum Mol Genet 10:537–543
Balemans W, Patel N, Ebeling M et al (2002) Identification of a 52 kb deletion downstream of the SOST gene in patients with van Buchem disease. J Med Genet 39:91–97
Loots GG, Kneissel M, Keller H et al (2005) Genomic deletion of a long-range bone enhancer misregulates sclerostin in Van Buchem disease. Genome Res 15:928–935
Gardner JC, van Bezooijen RL, Mervis B et al (2005) Bone mineral density in sclerosteosis; affected individuals and gene carriers. J Clin Endocrinol Metab 90:6392–6395
Wergedal JE, Veskovic K, Hellan M et al (2003) Patients with Van Buchem disease, an osteosclerotic genetic disease, have elevated bone formation markers, higher bone density, and greater derived polar moment of inertia than normal. J Clin Endocrinol Metab 88:5778–5783
Winkler DG, Sutherland MK, Geoghegan JC et al (2003) Osteocyte control of bone formation via sclerostin, a novel BMP antagonist. EMBO J 22:6267–6276
Van Bezooijen RL, Roelen BA, Visser A et al (2004) Sclerostin is an osteocyte-expressed negative regulator of bone formation, but not a classical BMP antagonist. J Exp Med 199:805–814
Poole KE, van Bezooijen RL, Loveridge N et al (2005) Sclerostin is a delayed secreted product of osteocytes that inhibits bone formation. FASEB J 19:1842–1844
Keller H, Kneissel M (2005) SOST is a target gene for PTH in bone. Bone 37:148–158
Robling AG, Bellido T, Turner CH (2006) Mechanical stimulation in vivo reduces osteocyte expression of sclerostin. J Musculoskelet Neuronal Interact 6:354
Li X, Zhang Y, Kang H et al (2005) Sclerostin binds to LRP5/6 and antagonizes canonical Wnt signalling. J Biol Chem 280:19883–19887
Hay E, Faucheu C, Suc-Royer I et al (2005) Interaction between LRP5 and Frat1 mediates the activation of the Wnt canonical pathway. J Biol Chem 280:13616–13623
Clement-Lacroix P, Ai M, Morvan F et al (2005) Lrp5-independent activation of Wnt signalling by lithium chloride increases bone formation and bone mass in mice. Proc Natl Acad Sci USA 102:17406–17411
Kulkarni NH, Onyia JE, Zeng Q et al (2006) Orally bioavailable GSK-3alpha/beta dual inhibitor increases markers of cellular differentiation in vitro and bone mass in vivo. J Bone Miner Res 21:910–920
Kulkarni NH, Wei T, Kumar A et al (2007) Changes in osteoblast, chondrocyte, and adipocyte lineages mediate the bone anabolic actions of PTH and small molecule GSK-3 inhibitor. J Cell Biochem 102(6):1504–1518
Glass DA II, Bialek P, Ahn JD et al (2005) Canonical Wnt signalling in differentiated osteoblasts controls osteoclast differentiation. Dev Cell 8:751–764
Holmen SL, Zylstra CR, Mukherjee A et al (2005) Essential role of beta-catenin in postnatal bone acquisition. J Biol Chem 280:21162–21168
Cohen P, Frame S (2001) The renaissance of GSK3. Nat Rev Mol Cell Biol 2:769–776
Harwood AJ (2001) Regulation of GSK-3: a cellular multiprocessor. Cell 105:821–824
Morvan F, Boulukos K, Clement-Lacroix P et al (2006) Deletion of a single allele of the Dkk1 gene leads to an increase in bone formation and bone mass. J Bone Miner Res 21:934–945
Tian E, Zhan F, Walker R et al (2003) The role of the Wnt-signalling antagonist DKK1 in the development of osteolytic lesions in multiple myeloma. N Engl J Med 349:2483–2494
Yaccoby S, Ling W, Zhan F et al (2007) Antibody-based inhibition of DKK1 suppresses tumor-induced bone resorption and multiple myeloma growth in vivo. Blood 109:2106–2111
Ott SM (2005) Sclerostin and Wnt signaling—the pathway to bone strength. J Clin Endocrinol Metab 90:6741–6743
Ominsky M, Stouch B, Doellgast G et al (2006) Administration of sclerostin monoclonal antibodies to female cynomolgus monkeys results in increased bone formation, bone mineral density and bone strength. J Bone Miner Res 21:S94
Padhi D, Stouch B, Jang G et al (2007) Anti-sclerostin antibody increases markers of bone formation in healthy postmenopausal women. J Bone Miner Res 22:S37
Silvestrini G, Ballanti P, Leopizzi M et al (2007) Effects of intermittent parathyroid hormone (PTH) administration on SOST mRNA and protein in rat bone. J Mol Histol 38:261–269
Van Bezooijen RL, ten Dijke P, Papapoulos SE, Lowik CW (2005) SOST/sclerostin, an osteocyte-derived negative regulator of bone formation. Cytokine Growth Factor Rev 16:319–327
Sutherland MK, Geoghegan JC, Yu C et al (2004) Sclerostin promotes the apoptosis of human osteoblastic cells: a novel regulation of bone formation. Bone 35:828–835
Leupin O, Kramer I, Collette NM et al (2007) Control of the SOST bone enhancer by PTH via MEF2 transcription factors. J Bone Miner Res 22(12):1957–1967
Brack AS, Conboy MJ, Roy S et al (2007) Increased Wnt signalling during aging alters muscle stem cell fate and increases fibrosis. Science 317:807–810
Liu H, Fergusson MM, Castilho RM et al (2007) Augmented Wnt signalling in a mammalian model of accelerated aging. Science 317:803–806
Holowacz T, Zeng L, Lassar AB (2006) Asymmetric localization of numb in the chick somite and the influence of myogenic signals. Dev Dyn 235:633–645
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Martin, T.J., Sims, N.A. & Ng, K.W. Regulatory pathways revealing new approaches to the development of anabolic drugs for osteoporosis. Osteoporos Int 19, 1125–1138 (2008). https://doi.org/10.1007/s00198-008-0575-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-008-0575-5